The flu shot

1. There is a 65% increase in the risk of non-influenza respiratory disease in influenza vaccinated populations
Although some studies suggest positive effects of the flu vaccine on the incidence of illnesses caused by flu viruses, that benefit is potentially outweighed by the negative effects of the flu vaccine on the incidence of non-flu respiratory diseases.1 To address patient concern that the flu vaccine causes illness (e.g. acute respiratory illness), the CDC funded a three-year study,2 published in Vaccine, to analyze disease risk after influenza vaccination versus disease risk in unvaccinated individuals.
The study, which included healthy subjects, found a 65% increase in the risk of acute non-flu respiratory disease within 14 days of receiving the flu vaccine. The authors state: "Patients' disease experiences after vaccination can be validated by these findings." The most common non-influenza pathogens found were rhinovirus, enterovirus, respiratory syncytial virus, and coronavirus.
This is important because, although flu vaccines target three or four strains of flu viruses,3 over 200 different viruses cause illnesses that produce the same symptoms - fever, headache, aches, cough and runny nose - of the flu4 and over 85% of acute respiratory illnesses are not related to the flu.5
2. Studies show that the flu shot does not reduce hospital demand
The National Institute of Health (NIH) funded a study6 to measure the effect of seasonal influenza vaccination on hospitalization of the elderly. The study analyzed 170 million episodes of medical care and found that "no evidence indicates that vaccination reduced hospitalizations."
Also, a 2018 Cochrane review7 of 52 clinical trials evaluating the efficacy of influenza vaccines found no significant difference in hospitalizations between vaccinated and unvaccinated adults. On the contrary, the reviewers found "Low certainty evidence that hospitalization rates and absence from work may be comparable between vaccinated and unvaccinated adults."
Additionally, the Mayo Clinic conducted a case-control study8 to analyze the effectiveness of the inactivated trivalent influenza vaccine (TIV) in preventing hospitalization for influenza in children aged 6 months to 18 years. The study evaluated the risk of hospitalization in vaccinated and unvaccinated children over a period of eight years. The authors state that: "TIV is not effective in preventing laboratory-confirmed influenza-related hospitalization in children." In reverse, "we found a three times higher risk of hospitalization in subjects who received the TIV vaccine".
3. Studies show that the flu vaccine does not prevent the spread of the flu
Families are believed to play an important role in the spread of influenza in the community, and families have long been analyzed to study the incidence and transmission of respiratory diseases of all severities. For this reason, the CDC funded a study9 on 1.441 participants, vaccinated and not, in 328 families. The study evaluated the ability of the influenza vaccine to prevent community-acquired influenza (domestic index cases) and acquired influenza in people with confirmed family exposure to influenza (secondary cases). Transmission risks were determined and characterized.
In conclusion, the authors state that: "There is no evidence that vaccination prevents home transmission once the flu is introduced."9,10
Also, a systematic review5 of 50 flu vaccine studies conducted for the Cochrane Library states that: "Flu vaccines have a modest effect in reducing flu symptoms and lost workdays. There is no evidence that they influence complications, such as pneumonia, or transmission. ".
4. The flu shot fails to prevent the flu about 65% of the time
The CDC conducts studies to evaluate the effects of flu vaccination with each flu season to determine if flu vaccines are working as intended.11 Since circulating influenza viruses are constantly changing (mainly due to antigenic mutations),12 flu vaccines are regularly re-formulated based on a "best guess" of which viruses might circulate during the next flu season.3 The CDC states that: "The CDC monitors vaccine efficacy annually through the Influenza Vaccine Effectiveness (VE) Network, a collaboration with participating institutions in five geographic locations ... [Annual vaccine efficacy estimates give a real idea of how far the vaccine protects against the flu caused by the viruses circulating every season ".13
Data from the CDC's Influenza VE Network indicates a vaccine failure rate of 65% between 2014 and 2018 (Fig. 1).11
Influenza vaccine failure
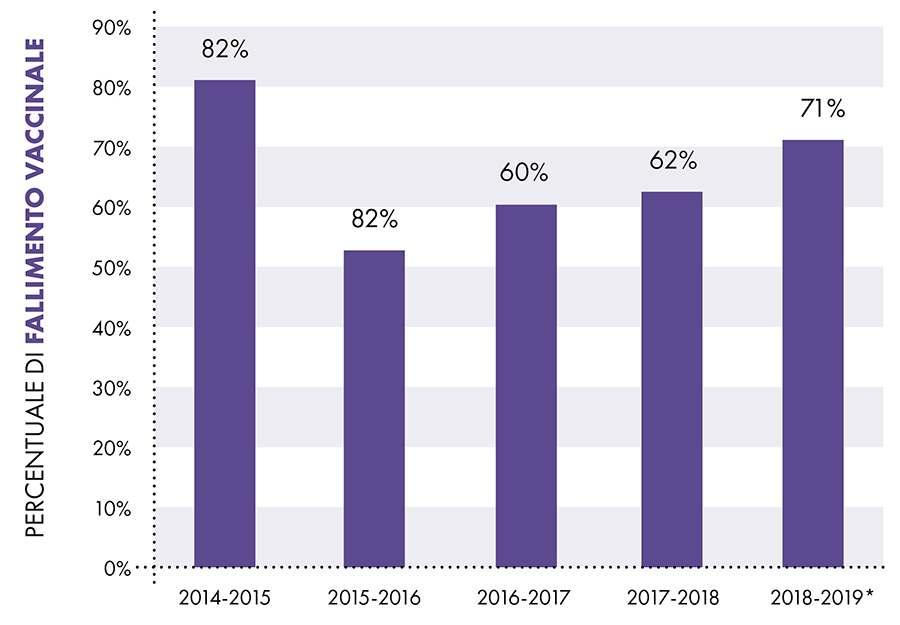
Figure 1: Data from the Centers for Disease Control and Prevention (CDC) of the US Flu VE Network indicates that the flu vaccine failed to prevent flu in 65% of cases.
5. Repeated doses of flu vaccine may increase the risk of flu vaccine failure
Some studies have observed that flu vaccines have low efficacy in people vaccinated for two consecutive years.9 A review of 17 flu vaccine studies published in Expert Review of Vaccines states: "The effects of repeated annual vaccination on long-term individual protection, population immunity and virus evolution remain largely unknown.".14
6. Death from flu is rare in children
Before the spread of the flu vaccine in children between 2000 and 2003, children aged 18 and under each year had about one in 1,26 million or 0,00008% chance of dying at cause of the flu.15 In a 2004 report, the CDC stated: "Influenza-related deaths are infrequent among children with and without high-risk conditions."16
7. Studies show that the flu shot does not reduce deaths from pneumonia and flu
The National Vaccine Program Office, a division of the United States Department of Health and Human Services (HHS), funded a study17 to examine flu mortality over 33 years (1968-2001). The study found no decrease in influenza mortality associated with widespread use of the flu vaccine. The authors state that: "We have not been able to correlate the increase in vaccination coverage after 1980 with the decrease in mortality rates in any age group ... [We conclude that observational studies substantially overestimate the benefit of vaccination ".
Additionally, the National Institute of Health (NIH) funded a study6 to measure the effect of seasonal influenza vaccination on elderly mortality. The study analyzed 7,6 million deaths and found "a sharp increase in influenza vaccination rates at the age of 65 without a corresponding decrease in hospitalization or death rates".
8. Studies show that patients derive no benefit from vaccinating healthcare professionals
A revision18 of over 30 flu vaccine studies conducted for the Cochrane Library states: "The results of our review did not identify conclusive evidence of the benefit of healthcare workers' vaccination programs on the specific outcomes of laboratory-proven influenza, its complications (lower respiratory tract infection, hospitalization or death from lower respiratory tract disease). or on all-cause mortality in people over the age of 60 ". The authors conclude: "This review does not provide reasonable evidence to support vaccination of healthcare workers to prevent influenza.". Furthermore, "There is little evidence to justify the requirement for medical staff to have influenza vaccination by doctors and public health workers".
9. The mandatory nature of the influenza vaccine is not based on science
A Cochrane Vaccines Field analysis19 evaluated studies measuring the benefits of flu vaccination. The analysis, published in the BMJ, concludes that: "The large gap between policy and what the data tells us (when rigorously assembled and evaluated) is striking ... Evidence from systematic reviews shows that inactivated vaccines have little or no effect on measured effects ... The reasons of the current gap between policy and evidence is unclear, but given the enormous resources involved, a reassessment should be undertaken urgently. ".
References
- Dierig A, Heron LG, Lambert SB, Yin JK, Leask J, Chow MY, Sloots TP, Nissen MD, Ridda I, Booy R. Epidemiology of respiratory viral infections in children enrolled in a study of influenza vaccine effectiveness. Influence Other Respir Viruses. 2014 May; 8 (3): 293-301. Epub 2014 Jan 31.
- Rikin S, Jia H, Vargas CY, Castellanos de Belliard Y, Reed C, LaRussa P, Larson EL, Saiman L, Stockwell MS. Assessment of temporally related acute respiratory illness following influenza vaccination. Vaccine. 2018 Apr 5; 36 (15): 1958-64.
- Centers for Disease Control and Prevention. Washington, DC: US Department of Health and Human Services. Selecting viruses for the seasonal influenza vaccine; [cited 2020 Aug 17]. https://www.cdc.gov/flu/prevent/vaccine-selection.htm.
- Demicheli V, Jefferson T, Al-Ansary LA, Ferroni E, Rivetti A, Di Pietrantonj C. Vaccines for preventing influenza in healthy adults. Cochrane Database of Syst Rev. 2014 Mar 13; (3): CD001269.
- Jefferson T, Di Pietrantonj C, Rivetti A, Bawazeer GA, Al-Ansary LA, Ferroni E. Vaccines for preventing influenza in healthy adults. Cochrane Database Sys Rev. 2010 Jul 7; (7): CD001269.
- Anderson ML, Dobkin C, Gorry D. The effect of influenza vaccination for the elderly on hospitalization and mortality: an observational study with a regression discontinuity design. Ann Intern Med. 2020 Apr 7; 172 (7): 445-52.
- Demicheli V, Jefferson T, Ferroni E, Rivetti A, Di Pietrantonj C. Vaccines for preventing influenza in healthy adults. Cochrane Database Syst Rev. 2018 Feb 1; 2 (2): CD001269.
- Joshi AY, Iyer VN, Hartz MF, Patel AM, Li JT. Effectiveness of trivalent inactivated influenza vaccine in influenza-related hospitalization in children: a case-control study. Allergy Asthma Proc. 2012 Mar-Apr; 33 (2): e23-7.
- Ohmit SE, Petrie JG, Malosh RE, Cowling BJ, Thompson MG, Shay DK, Monto AS. Influenza vaccine effectiveness in the community and the household. Clin Infect Dis. 2013 May; 56 (10): 1363.
- Physicians for Informed Consent. Newport Beach (CA): Physicians for Informed Consent. Vaccines: what about immunocompromised schoolchildren? Dec 2019. https://physiciansforinformedconsent.org/immunocompromised-schoolchildren/rgis/.
- Centers for Disease Control and Prevention. Washington, DC: US Department of Health and Human Services. CDC seasonal flu vaccine effectiveness studies; [cited 2020 Apr 17]. https://www.cdc.gov/flu/vaccines-work/effectiveness-studies.htm.
- Centers for Disease Control and Prevention. Washington, DC: US Department of Health and Human Services. How the flu virus can change: 'drift' and 'shift'; [cited 2020 Aug 17]. https://www.cdc.gov/flu/about/viruses/change.htm.
- Centers for Disease Control and Prevention. Washington, DC: US Department of Health and Human Services. How flu vaccine effectiveness and efficacy are measured; [cited 2020 May 14]. https://www.cdc.gov/flu/vaccines-work/effectivenessqa.htm.
- Belongia EA, Skowronski DM, McLean HQ, Chambers C, Sundaram ME, De Serres G. Repeated annual influenza vaccination and vaccine effectiveness: review of evidence. Expert Rev Vaccines. 2017 Jul; 16 (7): 723,733.
- Centers for Disease Control and Prevention. Washington, DC: US Department of Health and Human Services. CDC wonder: about underlying cause of death, 1999-2018; [cited 2020 May 2]. https://wonder.cdc.gov/ucd-icd10.html; queries for death from influenza, 2000-2003. Between 2000 and 2003, there were 61 annual deaths from influenza out of 77 million children age 18 and younger, about 1 death in 1.26 million.
- Harper SA, Fukuda K, Uyeki TM, Cox NJ, Bridges CB; Centers for Disease Control and Prevention (CDC) Advisory Committee on Immunization Practices (ACIP). Prevention and control of influenza: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep. 2004 May 28; 53 (RR-6): 1-40.
- Simonsen L, Reichert TA, Viboud C, Blackwelder WC, Taylor RJ, Miller MA. Impact of influenza vaccination on seasonal mortality in the US elderly population. Arch Intern Med. 2005 Feb 14; 165 (3): 265-72.
- Thomas RE, Jefferson T, Lasserson TJ. Influenza vaccination for healthcare workers who care for people aged 60 or older living in long-term care institutions. Cochrane Database Syst Rev. 2016 Jun 2; (6): CD005187.
- Jefferson T. Influenza vaccination: policy versus evidence. BMJ. 2006 Oct 28; 333 (7574): 912-5.
Article translated by Physicians for Informed Consent

